Coxarthrosis of the hip is a complex arthropathic pathology that leads to severe changes in the joint.Unfortunately, disabling disabilities in adults are common.In fact, according to statistics, hip joint disorders account for almost half of all disorders of the musculoskeletal system.I will give you a case of a rare complication after surgical treatment and during recovery.
Hip arthrosis: some knowledge about the disease
Osteoarthritis is a degenerative dystrophic change that causes complete destruction of cartilage and results in loss of joint function.
Hip Arthrosis - Here the hip joint is destroyed, actually, this is the same joint disease.
In terms of its mechanism, the hip-pelvis joint is similar to a door hinge.The femoral head is connected to the ischium like a hinge.There is a special anatomical structure - the acetabulum.This structure ensures maximum joint mobility.It performs a complete cycle of motion, or rather, flexion, extension, rotation, etc.
Under normal circumstances, the joint surface is smooth and there is enough fluid inside to ensure unimpeded sliding.As the disease progresses, the lubricant becomes thicker and more viscous, which immediately affects the condition of the cartilage.The synovial fluid no longer fully performs its functions.As a result, the shock pads can dry out, crack, and become rough.
- first.Due to the lack of necessary sliding, friction on the bones increases, causing bone injuries.
- second.As it progresses, deformation of the bone surface also connects with the altered cartilage tissue.Therefore, the body attempts to compensate for the increased load.
- third.Increased loading results in complete atrophy of the femoral muscles and weakness of the ligaments.
Important: Hip osteoarthritis is a progressive disease.Changes may cause a person to completely lose physical activity.ultimately leading to disability.And completely disrupted the usual way of life.The disease and its treatment are not only of great medical importance but also a major social problem.
Causes and types of hip arthritis
There is no definite cause of coxarthrosis (destruction of the hip joint), at least yet.There are only assumptions.Most cases of hip pathology development are associated with congenital hip dislocation and joint dysplasia (disadvantage).
Therefore, there are two types of hip arthrosis:
- Primary (caused by unknown cause);
- Secondary (related to injury, illness).
Primary osteoarthritis is characterized by a combination of factors:
- genetics;
- Effects of biological and mechanical processes;
- being overweight;
- Metabolic disorders;
- Yet another theory concerns pathological tissue repair in response to damaging factors (inflammation, friction, infection).
This type of hip arthropathy is often accompanied by spinal injuries and inflammatory phenomena in the knee joints (arthritis, arthropathy).
In the second version, the reasons for the development are clearer.These include:
- Dysplastic diseases.Grade 1 hip dysplasia occurs in half of all cases of congenital pathology.
- Hip dislocation (congenital).
- Life trauma.Fractures, dislocations, and subluxations of the pelvis and femoral neck.
- Legg-Calvé-Perthes disease.Development of osteochondrosis of the femoral head and its necrosis.This disease occurs in children when the blood supply and nutrients to the joints are compromised.
Furthermore, pathology can affect both modalities simultaneously or be unilateral.In addition to the direct causes of occurrence, there are predisposing factors that induce the development of the disease.This disease usually occurs as the load on an athlete's limbs increases.and people with difficult physical working conditions.Being overweight significantly increases the likelihood of joint disease.
Triggering factors also include:
- Disruption of metabolic processes, joint nutrition, hormonal imbalances.
- Lack of motivation.
- Bad posture.Scoliosis and kyphosis, in particular, can lead to misalignment of the pelvic bones.
- Age after 40 years old.It is estimated that after this date, 1 in 10 patients will be diagnosed with grade 1, 2 hip arthropathy.After the age of 60, one in every three people is observed.And by the time they were 70 or older, almost 80 percent of applicants had the condition.
No specific genes are responsible for the transmission of pathological changes in joints.However, genetic factors can still be traced.A person can obtain information on structural characteristics of cartilage tissue, metabolic changes, and bone pathology from relatives.It is this combination of genetic information that causes the hip joint to appear.
Classification
The disease is primarily classified according to severity.There are 3 stages, and not only are the symptoms different, but so are the changes on X-rays.It is these indicators that serve as the basis for diagnosis.
Bachelor of Science |
logo |
|---|---|
I |
|
two |
|
three, |
|
This division is the most common.There are also many types of Kellgren classifications.It consists of 4 stages, plus zero degrees - equivalent to healthy joints.
symptom
The basis of all diseases of the musculoskeletal system is pain.Symptoms of hip arthrosis in degrees 1-2 are less pronounced than in late stage 3.Initially, the pain will manifest itself during movement.Especially after a long walk or climbing stairs.Later, pain became a constant companion, significantly worsening quality of life.
Grade 1 hip arthropathy
The unpleasant sensation is concentrated only in the joint area (the groin and buttocks are almost unaffected) and is rarely reflected in the hips or knees.The pain may be relieved with rest.
At this stage, no further manifestations were detected - the gait remained unchanged and there were no movement disorders.In the dysplastic variant, on the contrary, there is an increase in mobility due to changes in the connective tissue; often in the initial stages of the disease, due to increased flexibility, patients become interested in gymnastics and yoga.Movement problems only occur in stage 3.
Symptoms of stage 1 hip arthrosis can be treated without surgery.Proper treatment can allow you to eliminate unpleasant symptoms and stop the progression of the disease.
Grade 2 disease
The pain, although not constant, is present at rest.Irradiation becomes evident - buttocks, groin, knees.Stiffness is observed - limitation of lifting movements, attempts to abduct to the side, difficulty in circular movements of the legs (pain especially often increases).Lameness becomes apparent after strenuous walking or running.
When moving, you will hear the characteristic crunching sound of the joint - rough and dry.
3rd degree osteoarthritis
The pain becomes constant and does not go away with rest and sleep.Even at night, unpleasant sensations do not leave the patient.Have difficulty walking; you must use crutches to move easily.The lameness is constant.
During this stage, the muscles in the limbs atrophy and the legs themselves become shorter.These changes force the patient to bend toward the affected side, further increasing the load on the joint.Restrictions on mobility were observed in almost all directions.
Bilateral Hip Changes in the hip joints alter the patient's gait, which is why all morphologies involved in walking are affected.Low back pain, posture disorder, and changes in pelvic axial position occur.
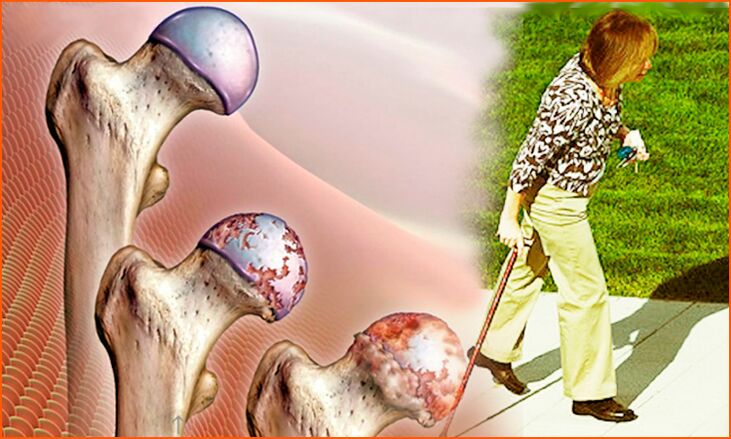
diagnosis
Examination by an orthopedic surgeon and a thorough analysis of the chief complaint play an important role in determining the disease.It is worth assessing the patient's activities - ability to climb stairs, comfort when wearing boots and socks, walking activities, use of crutches.
It is recommended to check general conditions - blood test, urine test, biochemistry, electrocardiogram, HIV marker measurement and syphilis.
Symptoms of 1st degree hip coxaarthrosis are the most subtle.That’s why it’s worth getting an X-ray to see changes in the joint space.This approach goes beyond identifying disease.And the cause of the occurrence is often found - dysplasia, Perthes disease.
Typically, knee pain is more pronounced in grade 1 hip deforming coxarthrosis, so this should be distinguished from knee arthropathy.The differential diagnosis also includes spinal examination to rule out radiculopathy (which causes radiating pain to the hips and knees).
In suspicious cases, MRI (allows you to examine soft tissue in detail) and CT (checks bone formation) are used.
treat
There is no complete cure for this disease, but modern medicine can restore lost mobility so you can live a full life.
Grade 1-2 disease is effective with physical therapy and medication.In the final stages, only surgery can help.In other cases, surgery is performed if the conservative treatments used do not relieve symptoms.
Treatment Level 1
Unfortunately, it is impossible to completely eliminate the pathology.For grade 1, treatment is aimed at stabilizing the condition.
During treatment, some general recommendations must be followed:
- Normalization of physical activity - it is recommended to reduce excessive stress (long hikes, running, jumping).
- Use shoes with good shock-absorbing soles and specialized insoles.
- lose weight.
- Mandatory physical therapy.
Important note: Many patients completely refuse gymnastics and any exercise due to pain.This is often associated with concerns about the possibility of increased pain and worsening of the condition.Practice has proven this belief wrong - regular exercise therapy can help strengthen muscles, prevent muscle atrophy, reduce pain and improve joint function.
There is no prescribed diet for grade 1 hip joint disease; moderate nutrition is prescribed for weight loss.It is also useful to add gelatin-containing products, canned fish with bones, and dairy products to your diet.
conservative
Use nonsteroidal anti-inflammatory drugs as a pharmaceutical approach.Due to the many side effects, medication is recommended to treat severe pain.You can combine them with a stomach protectant.
Ongoing pain can be relieved with intra-articular steroid injections, and painkillers may also be used.
To support, the following is provided:
- Muscle Relaxant – Relieves tension and relieves leg pain.
- Chondroprotectant – Improves the repair of cartilage tissue.
- Vasodilator (niacin) - Helps relieve vasospasm and increases tissue microcirculation.
Heat can also be used in combination (traditional treatments can also be used).They provide no therapeutic benefits but can help relieve muscle spasms.
Be sure to use physical therapy - UHF, magnet therapy, induction current, massage.
hip replacement surgery
To regain freedom of movement and relieve severe pain in the third stage, the patient was prepared for planned prosthetic surgery.This was a special operation to replace a destroyed formation with an artificial formation.These interventions completely restored the patient's mobility.Helping you completely return to your normal lifestyle.
Depending on the extent of the surgery, the prosthesis can be monopolar (only the worn femoral head is replaced) or bipolar (the surface of the acetabulum is also changed).Rehabilitation treatment is necessary after surgery so that the patient can return to an active life as quickly as possible.
For patients over 60 years old, a recovery period is planned before surgical treatment, allowing the recovery process to be completed in a shorter time.Artificial joints have a lifespan of approximately 20 years, but it's important to follow these recommendations:
- Exclude running, long distance walking, and jumping.
- Avoid lifting heavy objects.
- Avoid being in excessively forced static positions (especially for people who work while standing).
life events
My friend's husband needed endoprosthetic surgery.He was not diagnosed with hip arthritis but had a successful lumbar hernia removal.My condition didn't improve, so the tests continued, and when the problem was finally found, they arranged for me to have surgery.
After the replacement, everything came back safely, but the second hip also required surgical intervention.A year later, the surgery was repeated and successful.Then, from the first minutes after anesthesia, recovery and strict compliance with the doctor's recommendations are required.
What about our friends?On the way home from the hospital, I started to put pressure on my prosthetic joint (sitting for a long time and stepping on my foot).I had forgotten how careful I was the first time.As a result, the ligaments and muscles that don't have time to adjust to the implant can't hold it in place, and it pops out.
Of course, they inserted it, put a cast on it, and everything seemed fine.But he complained that he couldn't move his legs to the side, was in pain, and felt uncomfortable when walking.Although he developed both joints through exercises and various exercises, it was also a desire to work and move independently.
prevention
We have discussed the symptoms and treatment of coxarthrosis of the hip and its stages.
- Only daily physical activity can help you avoid serious complications and live to an advanced age without crutches.During Soviet times, serious work was carried out to prevent diseases of the musculoskeletal system and strengthen the immune system.It is difficult to recover the lost experience now. I know it very well, but I am too lazy to do it.
- Excess weight can wear down your joints to the point of embarrassment; endoprostheses are better but won't shed the extra pounds.My friend was so convinced of this that he didn't even try to eat less sweets and starchy foods.Proper nutrition is very important.
- I think lifting weights is bad for the entire skeleton as well.
- Bad habits (alcohol, smoking) remove calcium, magnesium and other beneficial substances from the body.
Just dig in and everything is connected.
Exercise every day and take care of yourself and your joints!
























